Last updated on November 11th, 2023
In the realm of dental restoration, titanium dental implants stand as a testament to modern medical innovation, offering a solution to the age-old problem of missing teeth. These implants, surgically inserted into the jawbone, represent more than just a cosmetic fix; they are a blend of science, art, and engineering. This blog post delves into the fascinating world of titanium dental implants, unraveling their significance, the science behind their use, and their impact on dental health and aesthetics.
Titanium, known for its strength and biocompatibility, has emerged as the material of choice in this field. We will explore why titanium is preferred over other materials, its unique properties, and how these contribute to the success of dental implants. From biocompatibility to osseointegration, each aspect of titanium’s role in dental implants reveals a layer of complexity and innovation.
Additionally, the post will cover the types of titanium used in dental implants, each with its specific properties and applications. Understanding these differences is crucial for both dental professionals and patients, as it directly impacts the success and longevity of the implants.
But like any medical procedure, titanium dental implants come with their own set of considerations. We’ll discuss the procedure, potential side effects, and how to recognize signs of complications. Moreover, we will weigh the pros and cons of titanium implants against their ceramic counterparts, helping patients make informed decisions based on their specific needs and conditions.
Finally, this post addresses frequently asked questions about titanium dental implants. From costs and longevity to their interaction with medical devices and airport security, we aim to clarify common queries and misconceptions.
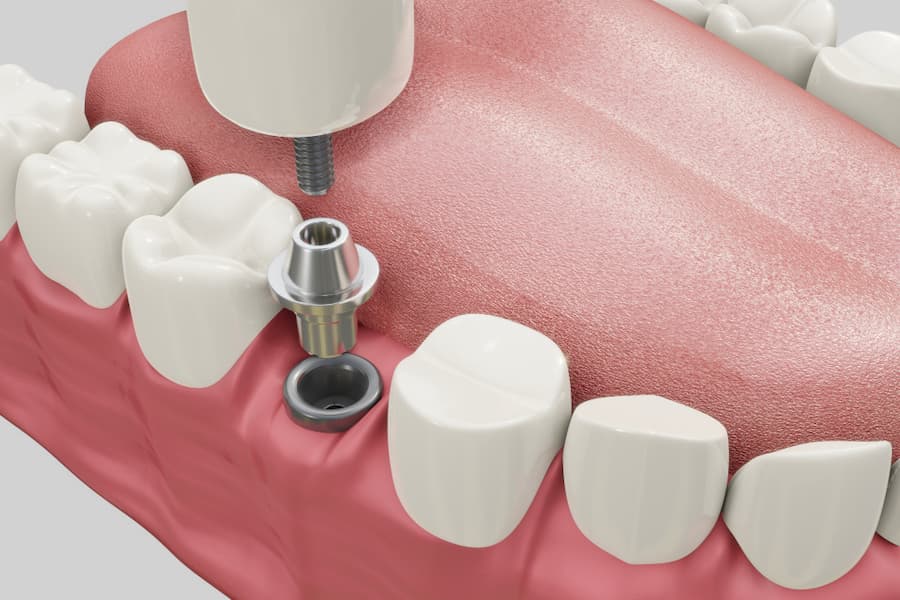
What Are Titanium Dental Implants?
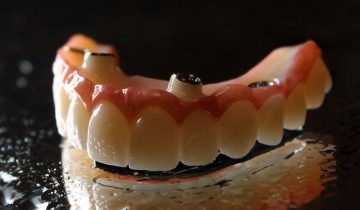
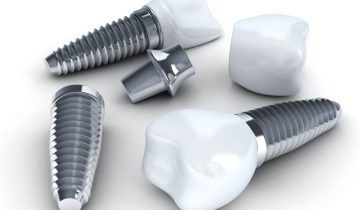
Titanium dental implants are a popular and effective way to replace missing teeth. They are surgically inserted into the jawbone and fuse with the bone over time, creating a strong and stable foundation for a replacement tooth or bridge. Unlike subperiosteal implants, titanium implants are endosteal anchors that support the bone structure and, of course, the crown attached to it. Numerous companies and brands manufacture titanium implants such as Nobel Biocare, Hiossen, Zimmer, or Strauman. .
Why Is Titanium Used For Dental Implants?
Titanium is the most widely used material for dental implants due to its remarkable properties that make it well-suited for this application. According to the study “Quality of Dental Implants” published in the International Dental Journal, “implants made from titanium and titanium alloys appear to perform well clinically in properly surgically prepared bone, regardless of small variations of shapes and forms.” Here are some of the key reasons why titanium is the preferred choice for dental implants:
- Biocompatibility: Titanium is considered a biocompatible material, meaning it can coexist peacefully with living tissue without causing adverse reactions. This property is crucial for dental implants, as they need to integrate seamlessly with the surrounding jawbone to provide a stable foundation for artificial teeth.
- Osseointegration: Titanium has a unique ability to bond with bone tissue, a process known as osseointegration. This remarkable phenomenon allows the implant to fuse with the jawbone, creating a strong and durable anchor that can withstand the forces of chewing and biting.
- Corrosion Resistance: Titanium is highly resistant to corrosion, which is essential for dental implants as they are constantly exposed to saliva, food particles, and other potentially corrosive substances. The inert nature of titanium ensures that the implant will not degrade or release harmful substances into the surrounding tissues.
- Strength and Durability: Titanium is a strong and durable metal that can withstand the stresses and strains of everyday use. This makes it an ideal material for dental implants, as they need to endure the forces of chewing, biting, and other oral activities without fracturing or breaking.
- Bioactive Surface: Titanium forms a thin oxide layer on its surface when exposed to air, which further enhances its biocompatibility and osseointegration properties. This bioactive surface promotes bone growth and attachment, facilitating the implant’s integration with the jawbone.
- Hypoallergenic Properties: Titanium is generally considered hypoallergenic, meaning it is unlikely to cause allergic reactions in most individuals. This makes it a safe choice for patients with metal allergies or sensitivities.
- Aesthetic Appeal: Titanium implants have a natural metallic appearance that blends well with the surrounding teeth and gums, contributing to a more aesthetically pleasing smile.
Actually, the use of titanium is not limited to dentistry. Doctors and medical technicians of various fields make use of titanium for a wide range of functions, such as spinal and bone fixators, artificial joints, bone conduction hearing aids, etc. Titanium is a common material used in medicine and dentistry due to its strong and safe nature.
What are the Types of Titanium Dental Implants?
Titanium implants are categorized into two main types:
- Commercially Pure Titanium (CPTi): CPTi is composed of 98-99.9% pure titanium, making it the most biocompatible and corrosion-resistant type of titanium. CPTi implants are typically used for dental and orthopedic applications due to their excellent biocompatibility and ability to bond with bone tissue.
- Titanium Alloys: Titanium alloys are formed by adding other elements to titanium to enhance its mechanical properties, such as strength, hardness, and ductility. Common titanium alloys used in implants include:
- Ti-6Al-4V: This alloy contains 6% aluminum and 4% vanadium, making it stronger and more wear-resistant than CPTi. Ti-6Al-4V is the most widely used titanium alloy for implants due to its excellent balance of strength, biocompatibility, and corrosion resistance.
- Ti-5Al-2.5Fe: This alloy contains 5% aluminum and 2.5% iron, offering similar strength to Ti-6Al-4V but with better ductility and workability. It is often used in orthopedic implants that require more flexibility.
- Ti-3Al-2.5V: This alloy contains 3% aluminum and 2.5% vanadium, providing a balance of strength, biocompatibility, and low density. It is often used in pediatric orthopedic implants due to its lightweight properties.
The choice of titanium implant material depends on the specific application and patient needs. CPTi is generally preferred for its biocompatibility, while titanium alloys are often chosen for their enhanced strength and durability. Factors like bone density, implant size, and expected load-bearing requirements also influence the material selection.
What is the Procedure of Titanium Dental Implant?
The procedure for placing titanium dental implants is a multi-step process that typically involves consultation and planning, implant placement, healing and osseointegration, abutment placement, and crown or bridge placement.
This illustration shows the dental implant procedure step by step.
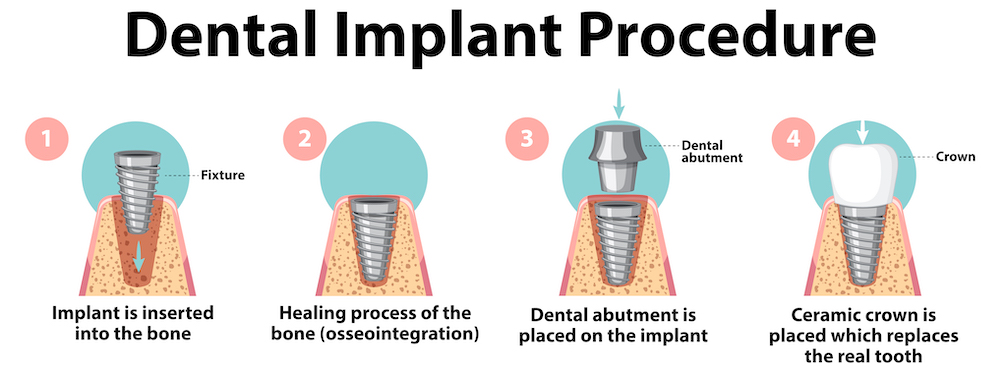
To learn more about the dental implant procedure, please visit the following blog post: Dental Implant Procedure
What are the Side Effects of Titanium Implants?
Titanium implants are are generally considered to be safe and effective, but like any medical procedure, there are some potential side effects that can occur. For example, the use of titanium dental implants may induce an allergic reaction such as facial eczema, according to the study “Suspected association of an allergic reaction with titanium dental implants: a clinical report” published in the Journal of Prosthetic Dentistry in 2008.
How Do You Know If Your Body Is Rejecting Titanium?
The following are the reported symptoms of titanium reactions in the body:
- Skin redness (erythema)
- Hives on the gum and outer skin (urticaria)
- Itchy inflammation on the skin (eczema)
- Pain or swelling
- Death of tissue around the implant area (necrosis)
- Toxic reactions like yellow nail syndrome
- Bone loss
You should immediately see your dentist if you experience any of these reactions.
When to Choose Ceramic versus Titanium Dental Implants?
Patients who are concerned about the visibility of the implant due to having thin gum tissue or gum recession prefer ceramic dental implants (zirconia) to titanium. Since ceramic dental implants are white, they can be more aesthetically pleasing when visible.
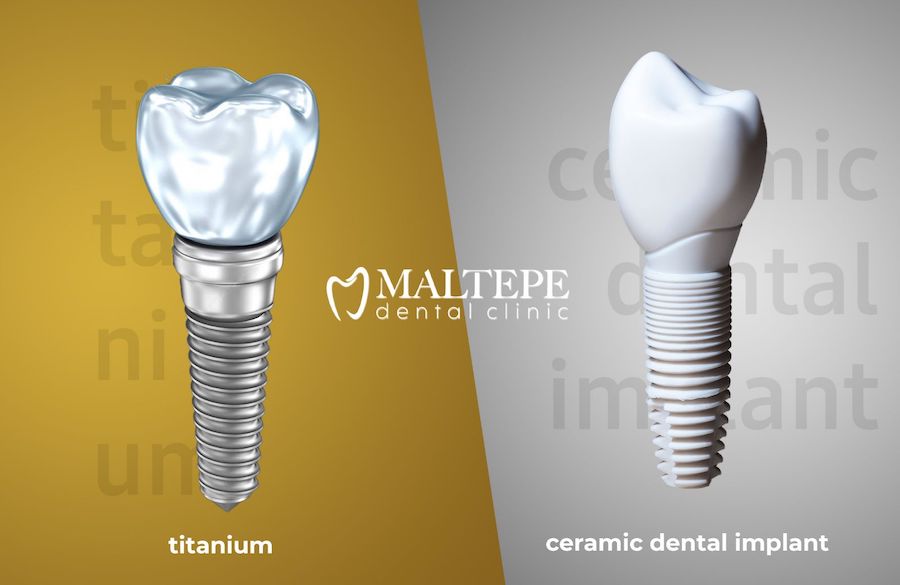
Ceramic implants also attract and retain fewer bacteria compared to titanium implants. This means potentially less inflammation. Moreover, the osseointegration rates of ceramic dental implants are similar to that of titanium.
On the other hand, ceramic implants are not used as widely as titanium implants. The clinical indications are therefore limited. Also, the manufacturing of ceramic implants can greatly impact the quality and price. For this reason, patients should thoroughly discuss their options with dental professionals.
FAQs About Titanium Dental Implants
Titanium dental implants have been used for a long time, but there may still be some points to clarify for those who are not at all familiar with them. Here are some of the most common questions and answers about titanium dental implants.
How Much Does A Titanium Dental Implant Cost?
The cost of a titanium tooth implant can vary between $2,000 and $6,000. The price can go higher depending on the prerequisite treatments.
How Long Do Titanium Dental Implants Last?
Titanium implants are well known for their durability and biocompatibility. With proper care, they can last for many years, often up to 25 years or even longer. The titanium screw itself, which fuses with the jawbone, is likely to last a lifetime. However, the dental crown, which is the visible part of the implant, may need to be replaced every 5 to 15 years.
Which Dental Implant Brands Manufacture Titanium Implants?
Numerous companies such as Nobel Biocare, Hiossen, Zimmer, or Strauman manufacture titanium implants. For more information about dental impant brands please visit the following blog post: “Top 10 Dental Implant Brands“.
Will Titanium Dental Implants Trigger Airport Security?
Titanium implants will rarely trigger security alarms at an airport.
Do Titanium Dental Implants Set Off Metal Detectors?
Titanium implants will not set off most metal detectors.
Can You Have An MRI If You Have Titanium Dental Implants?
Yes, you can. According to the study published in the Journal of Archive of Plastic Surgery in 2019, titanium is not affected by MRIs, and it is safe to conduct MRIs on people with titanium implants.